Healthcare has long been among the earliest sectors to adopt technology at scale. National health record systems, rapid vaccine rollout programmes, continuous drug discovery pipelines, and early use of AI in diagnostics all reflect an industry that doesn’t just experiment with innovation but operationalises it.
That pattern is now extending further. In leading healthcare organisations, AI is not just confined to pilots or research environments. It is being embedded in clinical workflows, hospital operations, and wider healthcare system design. Within a highly regulated environment, it holds the potential to address some of healthcare’s most persistent challenges – cost pressures, patient experience, and operational efficiency – reshaping how care is delivered, coordinated, and sustained across entire systems.
What is emerging is not a uniform transformation, but a system in transition. Across Asia Pacific, healthcare organisations are moving at different speeds, but broadly along the same trajectory: from experimentation to structured adoption, to system-level integration. The gap between these stages is where both the constraint and opportunities for AI in healthcare now sits.
















Strategy Is Forming, Even As Execution Scales
Healthcare organisations in Asia Pacific tend to sit at two extremes: a set of leading-edge institutions that are actively embedding AI into strategy and operations, and a larger group that is still in early stages of exploration, planning, or fragmented adoption.
This distribution is reflected in current adoption roadmaps, where most organisations are still in transition rather than execution.
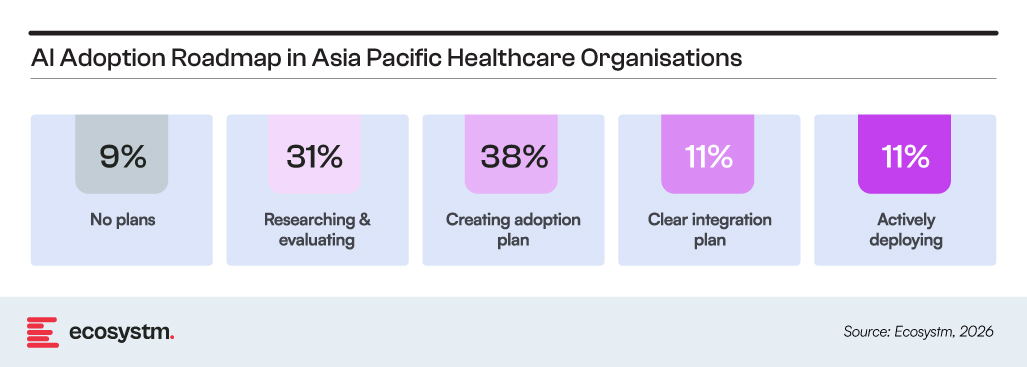
On one end, there are organisations with defined strategies, clear ownership, and early deployment across clinical and operational environments. On the other hand, many are still shaping direction, testing approaches, or building initial roadmaps without consistent execution.
AI has the potential to change the shape of this transition. When introduced deliberately and supported by the right infrastructure, regulatory alignment, and operating models, it allows healthcare providers to move beyond incremental maturity steps and accelerate towards system-level impact.
Adoption Concentrates Where Outcomes Are Immediate & Measurable
This two-speed pattern is also visible in how AI is being applied across healthcare organisations. Most activity is concentrated in areas where AI can be embedded into existing clinical and operational systems with clear links to care delivery, reliability, and system performance.
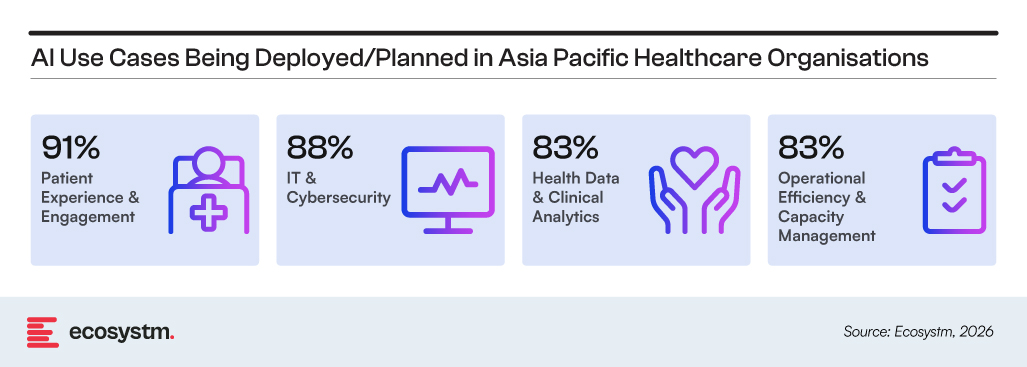
Patient experience and engagement is the most active area, with AI being used for triage support, virtual assistants, and more continuous care interactions beyond traditional point-of-care engagement. IT and cybersecurity sit alongside this as a foundational requirement, reflecting the need to maintain trust, safety, and continuity as healthcare systems become more digitised and interconnected.
As these capabilities mature, patient and operational data are increasingly being used to support more consistent clinical decision-making, stronger population-level insights, and improved coordination across care settings. At the same time, long-standing operational constraints such as demand planning, workforce allocation, and workflow coordination are being addressed through AI-enabled approaches designed to manage variability in demand and resource pressure more effectively.
Beyond these areas, adoption remains more uneven. Clinical research and innovation continue to lag, reflecting longer time horizons and higher complexity of implementation. Overall, organisations are prioritising areas where AI can be integrated into existing care and operational pathways, while more complex system-wide use cases evolve more gradually.
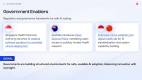
Governments Are Building The Regulatory & Data Foundations For Scale
Governments in Asia Pacific are focusing on the systems required to support safe and scalable AI adoption in healthcare.
In Singapore, the Health Sciences Authority has introduced an AI medical software sandbox to enable controlled deployment of lower-risk AI systems within public healthcare institutions. It allows selected solutions to be tested in real clinical environments without full regulatory licensing, but under strict safeguards including clinician oversight, institutional accountability, and mandatory patient notification. The approach is designed to balance innovation with patient safety while creating a pathway for eventual regulatory integration at scale.
Australia’s National Open Science Policy is pushing publicly funded health research towards greater transparency, requiring open access to research outputs, including data, methods, software, and code. The policy is aimed at improving collaboration and reducing duplication across the research ecosystem, while maintaining appropriate safeguards for intellectual property and sensitive population health contexts.
Cross-border collaboration is also expanding. Indonesia and China have established a joint digital health laboratory focused on AI in medicine, standardisation, and health system capability building. The initiative reflects a broader effort to strengthen domestic capacity while aligning with emerging global practices in digital health governance.
These developments reflect a shift towards building enabling environments for healthcare AI – through regulation, data access, and structured collaboration rather than isolated innovation.
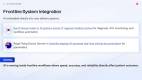
AI Is Being Embedded Into Frontline & Regional Care Delivery Systems
Healthcare systems are deploying AI directly into frontline and regional care environments, where clinical decisions, speed, and accuracy have immediate consequences for patient outcomes.
In South Korea, the Ministry of Health and Welfare is rolling out AI-based systems across all 17 regional medical centres. These systems support early detection of patient deterioration in intensive care units, assist in interpreting complex diagnostic imaging, and automate routine clinical documentation and administrative tasks, with the aim of improving both patient safety and operational efficiency across hospital networks.
In emergency care settings, the Royal Flying Doctor Service in Victoria is developing an AI-powered clinical documentation system for paramedics and transport teams. The system captures and structures patient information in real time during ambulance care, generating clinical summaries while reducing manual documentation in high-pressure environments.
In both examples, AI is not positioned as an external tool, but as part of the care delivery process itself, embedded into frontline workflows where reliability and timeliness are critical.
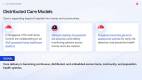
AI Is Extending Into Homes, Communities & Population Health Systems
Alongside hospital transformation, healthcare delivery is increasingly extending beyond traditional clinical settings into homes, community environments, and population health systems.
In Singapore, Home Control International and Nanyang Technological University are developing an AIoT-enabled home healthcare ecosystem that integrates monitoring, care coordination, and connected devices into a structured care platform. In Malaysia, Selangor is piloting AI-powered monitoring systems for elderly care across homes and care centres, using sensors and AI to detect falls and trigger real-time alerts for caregivers and families.
At the same time, countries are strengthening the underlying clinical and data foundations required to support this shift. Singapore’s genomic assessment centres are enabling earlier risk detection and preventive interventions, while India is applying large-scale AI models such as MedGemma in collaboration with medical institutions to support analysis of imaging and clinical data.
These drive a distributed healthcare model, where care is continuous, data-driven, and increasingly delivered across home, community, and system-wide networks rather than being anchored solely in hospitals.
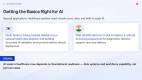
Healthcare Is Building The Foundations For AI At Scale
As AI adoption expands, focus is moving from standalone applications to the foundations required to make them work at scale – data readiness, system interoperability, compute capacity, and workforce capability.
In South Korea, efforts are underway to connect clinical datasets across hospitals into a centralised health and medical data platform, alongside structured environments to test and validate AI systems before deployment. The emphasis is on strengthening the underlying plumbing – reliable data flows, controlled validation, and system-wide readiness – rather than isolated use cases.
Capability is another foundational requirement. In India, more than 40,000 doctors have enrolled in a national AI training programme focused on diagnostics, decision support, and care delivery. The scale reflects a shift in reality: AI is moving into everyday clinical practice and requires broad-based clinical fluency, not specialist expertise alone.
These are indications of a more grounded phase of adoption, where the focus is on whether healthcare systems have the data foundations and workforce readiness to support AI at scale.
Ecosystm Opinion

Tech adoption within healthcare providers has rarely been straightforward. Legacy infrastructure, fragmented data exchange, poor interoperability, and organisational silos have traditionally limited the ability to scale technology consistently across clinical, administrative, and operations teams.
AI introduces flexible ways to work across fragmented systems and datasets, reducing some of the integration constraints that slowed earlier waves of digitisation. Combined with government-led efforts around data integration, governance, and infrastructure, this creates an opportunity for healthcare providers to move beyond incremental transformation and address structural limitations more directly.
FAQ: AI in Healthcare in Asia Pacific1. How is AI being used in healthcare today?
AI is being used across hospitals and health systems for diagnostics, patient engagement, clinical decision support, operations, and administrative workflows, with increasing integration into core clinical processes.
2. Is AI widely used in hospitals yet?
AI adoption is growing but uneven. While some leading healthcare organisations are embedding AI into operations, many are still in pilot, evaluation, or early adoption stages.
3. What are the main use cases of AI in healthcare?
Key use cases include patient triage and engagement, virtual assistants, clinical analytics, cybersecurity, operational efficiency, and capacity management.
4. Why is healthcare AI adoption still in early stages?
Adoption is constrained by fragmented data systems, legacy infrastructure, regulatory complexity, and challenges in scaling beyond pilots into enterprise-wide deployment.
5. How are governments supporting healthcare AI adoption?
Governments are enabling adoption through regulatory sandboxes, open science data policies, cross-border collaboration initiatives, and investments in national health data infrastructure.
6. How is patient data protected in healthcare AI systems?
Data protection approaches include privacy-by-design frameworks, data masking, regional data controls, governance standards, and regulated environments for AI testing and deployment.
7. What infrastructure is needed to scale AI in healthcare?
Scaling AI requires strong data infrastructure, interoperable systems, sufficient compute capacity, secure cloud environments, and robust governance frameworks.
8. How are doctors and healthcare workers using AI?
Healthcare workers are using AI for diagnostics, clinical decision support, documentation, research, and workflow optimisation, with increasing reliance on AI in day-to-day practice.
9. Is AI replacing doctors in healthcare?
No. AI is primarily augmenting clinicians by supporting decision-making, improving efficiency, and reducing administrative burden rather than replacing clinical roles.
10. What is the future of AI in healthcare systems?
Healthcare AI is moving toward system-wide integration, where care delivery, governance, infrastructure, and workforce capability are aligned to enable scalable, continuous, and data-driven healthcare systems.












